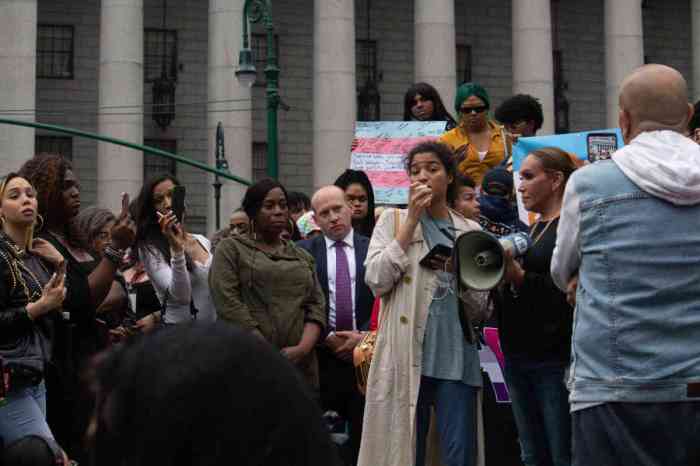Advocates show their support for reforming the New York State Medicaid program's policies regarding coverage of gender transition costs. | SRLP.ORG
A US district judge has granted summary judgment to four transgender plaintiffs on a claim that the New York State Medicaid program’s categorical ban on “cosmetic surgery” related to gender transition violates the federal program’s requirement to fund medically necessary treatment.
Judge Jed Rakoff’s July 5 ruling came on pre-trial motions in a lawsuit brought by a team of public interest and pro bono lawyers challenging the way New York’s program provides or withholds coverage for gender transition medications and procedures.
The ruling eliminates significant barriers many transgender adults have encountered in receiving Medicaid coverage for transition procedures their doctors find medically necessary but the state has deemed “cosmetic” and therefore not eligible for coverage.
US court finds blanket ban unlawfully blocks medically necessary procedures
Left open for further litigation, however, are important questions regarding Medicaid coverage in the case of minors.
The four plaintiffs, suing “on behalf of themselves and all others similarly situated,” challenged the exclusion of coverage for gender reassignment surgery and hormone therapy for individuals under age 18 as well as the regulation that imposes, according to Rakoff’s interpretation, “a blanket ban on coverage of cosmetic procedures related to gender dysphoria,” including procedures that the plaintiffs contend are “medically necessary” for their gender transition process.
Rakoff, last year, approved the plaintiffs’ motion for class action certification.
Dr. Howard Zucker, the commissioner of the State Department of Health and the named defendant in the suit, had asked the court to reconsider its prior decision against dismissing the cosmetic surgery claim, contending that the program does not actually have a “blanket ban” because it has occasionally approved coverage for particular procedures on a case-by-case basis.
Rakoff, however, concluded that regardless of any steps the department was taking to make exceptions, the written regulation is a blanket ban.
The judge also rejected Zucker’s motion to decertify the plaintiff class on the grounds that none of the named plaintiffs could represent the full range of issues presented by the proposed class. On this point, Rakoff found that “subclasses” could be created to deal with specific aspects of the case, but that there were enough common questions of law to justify retaining the class certification.
For many transgender people, Rakoff’s ruling that a blanket exclusion of coverage for cosmetic surgery regardless of medical necessity violates the Medicaid statute is the big news coming out of this decision, since the categorical ban presented a substantial barrier to individuals seeking comprehensive coverage for all the procedures they and their doctors deemed necessary to a full and successful transition.
However, on the question of providing therapy for minors, Rakoff concluded that there are significant factual disputes that prevented him from rendering a complete summary judgment. He ordered that the case proceed to trial on contested issues regarding both hormone therapy and surgical procedures.
An important question to be resolved is whether coverage for minors is limited to specific treatments spelled out in the federal government’s official compendium of approved drugs for use in treating gender dysphoria or if the Medicaid statute’s underlying requirement for coverage of all medically necessary therapy and procedures overrides the compendium’s limitations. Resolving this question will involve sorting out controversial issues related to what gender transition steps are appropriate for minors.
Plaintiffs are represented by attorneys from the Legal Aid Society and the Sylvia Rivera Law Project, as well as attorneys working pro bono. The New York Attorney General’s Office represents the Department of Health.
In a press statement, SRLP praised Rakoff’s ruling for finding “that the list of procedures New York State Medicaid had deemed suspicious or cosmetic was unlawful and that New York must provide Medicaid coverage for these procedures.”
The group also noted that the ruling “determined that SRLP and our colleagues at the Legal Aid Society and Willkie Farr & Gallagher LLP should become ready for trial on the issue of what types of treatments are medically necessary to treat gender dysphoria in individuals under the age of 18.”